In my years researching and writing about obesity, diabetes, medications, and the journey to better health, few developments have generated as much genuine hope—or as many questions—as the arrival of GLP-1 therapies for weight management. Among these, semaglutide has rapidly become a medication that people living with overweight or obesity discuss, investigate, and increasingly use under medical supervision.
This article brings my perspective on what I’ve learned and witnessed. My aim is to help you understand the science, practicalities, and risks—along with tips that make the difference between confusion and real, meaningful results. Tracking your journey with apps like Mingo can turn that difference into daily clarity and, as I’ve seen, a feeling of control that makes all the effort worthwhile.
Understanding GLP-1 and how it works for weight loss
When people ask me what GLP-1 is, I usually say it’s a “helper” hormone. GLP-1 stands for glucagon-like peptide-1, and its role in the body is to modulate appetite, prompt insulin after meals, and tell the brain, “I feel full.” These actions are fundamental to why GLP-1 therapies support both blood sugar control and weight loss.
Semaglutide is a medicine designed as a GLP-1 receptor agonist: it essentially mimics the effects of natural GLP-1, but in a way that can last longer and be more impactful than the body’s own short-lived hormone. This is how it works: after you inject semaglutide, it circulates in the blood, binding to specific receptors found in your pancreas and brain. There, it boosts the natural effect of GLP-1, helping to reduce hunger, slow stomach emptying, and prompt the pancreas to release more insulin only when blood sugar is high.
What I’ve noticed through patient stories and in published data is that these effects compound over time. It is not uncommon to see people, for the first time in years or even decades, experience genuine satiety and a marked decrease in food cravings. The urge to snack late at night, for example, gets weaker; impulsive eating becomes less frequent.
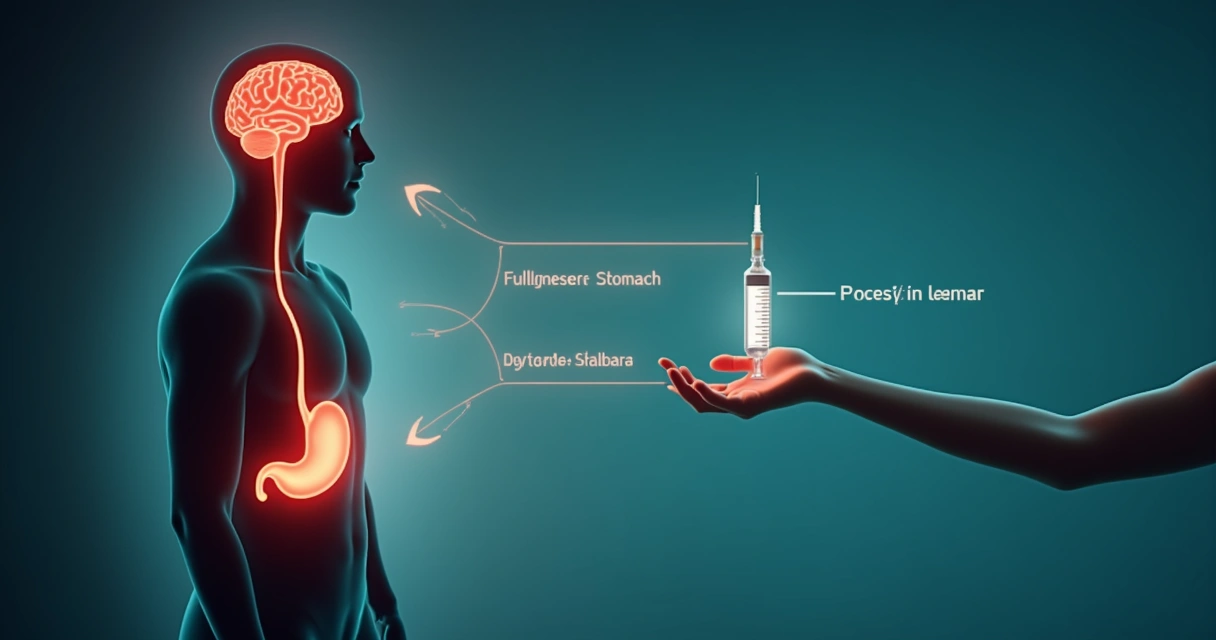
It isn’t just weight loss and appetite, though. Because GLP-1 therapies improve insulin sensitivity and promote the release of insulin only when the body needs it, they help stabilize blood sugar for people with type 2 diabetes as well. More on this connection can be found in my extended guides for GLP-1 users here.
The science: evidence on semaglutide and weight reduction
Clinical evidence makes it clear that substantial, healthy weight loss is possible with GLP-1 receptor agonists. Let’s talk data. A large randomized controlled trial of nearly 2,000 adults without diabetes found that weekly semaglutide injections at 2.4 mg led to an average weight reduction of 14.9% over 68 weeks, compared to just 2.4% for those on placebo. Strikingly, nearly one third of those treated achieved a loss of at least 20% of their initial body weight (study in PMC).
For many people, this is the first time true, durable weight loss feels real.
In practice, a retrospective study conducted by the Mayo Clinic on over 300 patients reported an average body weight reduction of 13.4% after one year, with meaningful improvements in cholesterol levels and blood pressure as well (summary here). The results are not limited to clinical trials—they are borne out in everyday life, too.
Another meta-analysis confirmed these effects, showing a mean weight loss just over 10% (approx. 10.5 kg), lower body mass index, and smaller waist circumference. The most common adverse reactions were gastrointestinal but were usually transient and manageable (systematic review data). You can find more in-depth guidance in my article on how semaglutide works at Mingo.
It’s also important to say that the trend holds in larger, real-world cohorts. As documented recently, people prescribed semaglutide in a routine clinical setting achieved a median weight reduction of 14.4% after 12 months (observational data).
Taken together, the science and anecdotal experience point in the same direction: semaglutide helps many people living with overweight or obesity reach meaningful, sustained weight loss, improve metabolic markers, and feel more control over their health.
Mechanism of action: what makes GLP-1 agonists unique?
What stands out for me, as both a researcher and communicator, is how this class of medicine achieves multiple effects through a single molecular pathway.
Semaglutide links to the GLP-1 receptor on cells in the pancreas and brain, which triggers a set of actions:
- Stimulates insulin production only when blood glucose is high, lowering risk of hypoglycemia
- Slows down stomach emptying, extending sensations of fullness after meals
- Suppresses glucagon (a hormone that raises blood sugar) after eating
- Reduces cravings and overall food intake via central appetite signals in the brain
Unlike some prior therapies, GLP-1 agonists do not increase the risk of low blood sugar unless combined with certain other diabetes medications. That’s why so many clinicians, myself included, recognize their far-reaching relevance—not only for weight but also for diabetes risk and cardiovascular health.
The connection: diabetes control and obesity treatment
It is easy to overlook, but semaglutide was initially developed for blood sugar management in type 2 diabetes, not obesity. The connection became apparent when patients began losing remarkable amounts of weight while under treatment for diabetes.
Now, semaglutide and other GLP-1 receptor agonists have proven, in repeated studies, to improve key health outcomes:
- Lower blood glucose and HbA1c for people with type 2 diabetes
- Promote significant, lasting weight loss for people with or without diabetes
- Reduce the risk of some major cardiovascular events in higher-risk groups
These findings have led major healthcare guidelines to recommend GLP-1 therapies as a cornerstone in modern metabolic care for obesity, provided they are used under medical supervision and as part of a broader health plan.
You can see a detailed overview of these linked benefits in my semaglutide weight loss guide.
Getting started: dosing schedules and adherence
Taking semaglutide is not like taking a daily pill. It is usually provided as a subcutaneous injection, most often once per week and at a fixed dose. Your doctor will typically begin with a lower starting dose (for example, 0.25 mg weekly), then “titrate” up over several weeks until the standard maintenance dose is reached—often 2.4 mg per week for weight management.
The gradual dose increase gives your body time to adjust.
For someone new to weekly injections, keeping track of the day and time for each dose is a real challenge. I recommend—both as a practical writer and an observer of countless journeys—a multi-layered remembrance system:
- Set recurring reminders in your phone or calendar
- Log each injection in an app like Mingo to generate a visual record
- Post a simple weekly mark, like a sticker or note, somewhere visible at home
If a dose is missed, take it as soon as you remember—unless it’s been more than five days, in which case skip and wait for your next scheduled injection. Do not double dose to make up for missed time; this is unsafe. The importance of these routines was echoed in multiple guidelines available in the latest World Health Organization recommendations for chronic GLP-1 therapy.
Tracking progress with digital tools: practical tips
While apps are everywhere these days, not all are designed for the unique needs of GLP-1 therapy users. An app like Mingo, developed specifically for people using semaglutide and related medications, streamlines the process. You can quickly log meals, symptoms, injection dates, and side effects—all of which build a clear picture over weeks and months.
In my experience, these logs transform bewilderment into insight: people start to notice triggers for stomach discomfort, find links between certain foods and nausea, or even patterns in their mood and energy across the cycle.
Small data builds big clarity.
Mingo also connects with tools like Apple Health, making it even less likely you’ll lose track. Recording details about water intake, protein, fiber, side effects, and even mood can help you and your healthcare provider adjust the plan before small problems become barriers. A great starting point for setting up tracking in your semaglutide journey is found in practical step-by-steps, such as the tips for weight loss with GLP-1 guide.
![]()
Tracking empowers users to spot trends, see progress, and communicate more effectively with healthcare professionals.
What to do if a dose is missed
This is a source of real anxiety, especially for people early in their GLP-1 journey. Here is how I recommend handling it, based on both guidelines and clinical practice:
- If missed and less than five days have passed, take the dose when you remember.
- If more than five days have passed, skip the missed dose and continue with your regular schedule.
- Never inject two doses together to try to compensate.
- Log the missed dose in your tracking app and alert your healthcare provider if you frequently miss doses, as adjustments may be needed.
These steps keep you within safety margins and maintain effective blood levels of the medication, reducing risk and frustration. If you find missed doses are common, it’s a signal to ask for support and find a reminder system that truly works for your lifestyle.
Common side effects and when to worry
Most people experience at least some degree of gastrointestinal symptoms. This is part of how semaglutide works—slowing stomach emptying can lead to nausea, bloating, or even mild vomiting, especially after larger meals or fatty foods.
The most common adverse reactions are:
- Nausea (most common, largely in the early weeks)
- Diarrhea
- Constipation
- Indigestion and sometimes mild abdominal pain
Most side effects fade within a few weeks as the body adapts.
For a smaller subset, symptoms like severe abdominal pain, persistent vomiting, jaundice (yellowing of eyes or skin), or changes in vision should prompt an immediate call to your health professional. Among the rare but serious risks discussed in clinical literature is a very low risk of pancreatitis (inflammation of the pancreas) and, in extremely rare cases, a condition called NAION (an eye disorder). The European Medicines Agency notes the latter to be less than one in 10,000 users and is still considered under investigation.

If you notice any unusual symptoms or those that alarm you, don’t ignore them—timely reporting can make all the difference in managing risks.
The risks of improper use: why prescription safety matters
I cannot stress this enough: obtaining semaglutide from unregulated or informal sources poses serious risks. Only a qualified healthcare provider can prescribe it safely, ensuring careful dose titration, side effect management, and ongoing monitoring for rare complications.
The active ingredient in GLP-1 agonists must be handled with strict regulatory oversight. Compounded or “off-market” versions, which sometimes appear online or through unofficial vendors, may carry variable dosages, impurities, or even completely incorrect substances. If the cost or access seems “too good to be true,” it’s a red flag—and the risk is not worth it. Major health authorities and the World Health Organization strongly advise against unsupervised or self-directed use of weight loss injectables.
Your safety lies in prescription-only, regulated medications.
Another major risk is the temptation to self-adjust the dose upward, under the impression that this will prompt faster results. In reality, excessive or mistimed dosing increases the risk of side effects and may blunt the intended effects by disrupting your body’s adaptation process.
Self-monitoring and the benefits of symptom, meal, and mood logging
It is clear to me that the more actively you log your food, symptoms, and mood while using semaglutide, the better your results will be. These records are more than a formality—they are the foundation of ongoing, effective care.
I have seen users, with the help of tracking, realize which foods trigger more nausea, which days are better for exercise, and what mood shifts appear as their body weight drops. Apps developed specifically for GLP-1 users, like Mingo, let people record details weekly, daily, or as needed without the friction of traditional pen and paper.
There’s another, crucial benefit: if troubling symptoms arise, a detailed log helps your healthcare team respond quickly and accurately. Patterns become clear, and decision-making is improved for both you and your care provider.
Tracking empowers you to take an active role in your GLP-1 therapy, transforming uncertainty into clear, constructive action.
Why buying from unregulated sources is never safe
There is a growing market for “gray area” or overseas versions of GLP-1 medications, sometimes promoted as affordable alternatives. This is particularly risky for injectables, where the wrong dose, poor quality, or inappropriate storage can be genuinely dangerous. These copycat products may contain incorrect ingredients, contaminants, or worse.
In my view and according to all major clinical guidelines, the health risk far outweighs any money saved by bypassing regulated, prescribed medication. Real semaglutide is available only by prescription, and pharmacy-based supply chains with medical support are the only sensible path for any injectable therapy.
Whenever I have spoken with patients who tried to use “compounded” or mail-order semaglutide analogs, their experiences range from ineffective to, at times, outright hazardous. You can find more detailed discussion of this risk in my earlier articles, where I interviewed pharmacists and endocrinologists with direct knowledge of these dangers.
The need for individualized medical supervision
No two journeys are the same. Some people experience rapid weight loss, while others progress more slowly. Differences in genetics, preexisting health conditions, diet adherence, and exercise all shape outcomes in unique ways.
That’s why every reputable guideline and specialist I know recommends individualized medical supervision when starting and adjusting GLP-1 therapy. Your doctor will screen for contraindications, set dosing schedules, and monitor both for effectiveness and side effects.
Supervision is your best protection against unexpected complications.
Part of this individualized approach is adapting dietary, movement, and sleep routines in concert with your changing appetite and body composition. This is another reason I recommend digital tools like Mingo—because a shared record between you, your healthcare team, and your daily life keeps everyone moving in the same direction.
How to monitor progress—and why logging matters for weight, wellbeing, and side effects
When I first started studying people’s real-world journeys with GLP-1 therapies, I noticed something: those who tracked not just weight, but also meals, emotional state, and medication side effects, were better able to adjust, stick with the program, and report higher satisfaction.
The act of logging makes progress tangible. It lets you see, at a glance, how much water you’ve been drinking, how many protein-rich meals you’ve had, or how your mood scores change as your body adapts. Periodic review—either on your own or during medical check-ins—turns small victories and potential setbacks into actionable guidance.
I often counsel people to set aside five minutes each week to review their app log—looking for connections between food choices, mood, and weight loss. If side effects or plateaus become apparent, this review is also a cue to seek further advice. Sharing these details with your doctor or nutritionist greatly magnifies the value of each visit and ensures concerns are quickly noticed and addressed.
Your health data is your power.
Why digital platforms like Mingo support effective GLP-1 use
The difference between a generic health tracking app and one purpose-built for semaglutide users matters more than you’d think. Mingo was created for the express purpose of bringing all the relevant metrics together: injection dates, meal and macro tracking, mood, hydration, protein, fiber, and side effect logging.
Data is stored locally for privacy, and, from what I hear users say, the interface is genuinely simple compared to more cluttered or technical options. The integration with Apple Health can also streamline syncing health records with permission, avoiding manual data entry.
For anyone embarking on their first clinical prescription or seeking to deepen their understanding after starting treatment, I firmly believe a tailored tool like Mingo acts as a bridge between hopes, outcomes, and everyday actions.
Putting it all together: a stepwise approach for success
Having talked to hundreds of people about their journeys with GLP-1 therapies, here’s how I’d sum up the most repeatable pattern for success:
- Start with a thorough medical assessment and clear, realistic discussion of goals.
- Follow your prescribed titration and dose schedule—don’t rush increases or skip medical visits.
- Track meals, injections, water, and side effects diligently using a secure digital record.
- Adapt your diet and movement routines to better align with new sensations of satiety and occasional GI symptoms.
- Communicate regularly with your care team, taking notes or screenshots from your app logs as needed.
- Address any cost or access barriers with your health provider, not with unregulated “alternatives.”
With individualized supervision, diligent tracking, safe medication supply, and the self-awareness that only logging brings, people using semaglutide can give themselves the very best chance at safe, lasting weight loss and improved metabolic health.
If this journey resonates—or if you’re considering taking the next step—I invite you to try out Mingo, see your own data unfold, and empower your journey with clarity and safety built right in.
Conclusion
In my experience, semaglutide is opening doors for many who have struggled with weight and metabolic health for years. Its mechanism of action, substantial evidence base, and growing clinical acceptance make it a compelling option—when used under proper supervision.
Digital tracking is the thread that brings everything together, whether capturing a good week or navigating side effects. The difference is real and, to my mind, transformative. Your health record is your own—turn it into your guide.
If you’d like to know more about Mingo, or want a tool that can simplify your journey with GLP-1 medications, I encourage you to begin today. Personalize your plan, secure your private data, and give yourself the support that successful long-term change deserves.
Frequently asked questions
What is semaglutide used for?
Semaglutide is prescribed to help adults manage chronic overweight and obesity, often alongside changes in diet and activity. It is also used to control blood sugar in people with type 2 diabetes. Its dual action provides significant benefits for weight management and glycemic control.
How does semaglutide help with weight loss?
Semaglutide mimics a natural hormone called GLP-1, which helps reduce appetite, slow down how quickly the stomach empties, and promote feelings of fullness. This triple effect leads to fewer calories consumed, lower cravings, and, over time, measurable weight loss. The medication’s ability to stabilize insulin and limit spikes in hunger is what makes it so effective for many users.
What are common side effects of semaglutide?
The most common side effects are gastrointestinal, especially nausea, diarrhea, constipation, and sometimes mild abdominal pain or indigestion. These tend to be most noticeable in the early weeks and generally fade as the body adapts. More severe, but rare, risks include pancreatitis and a very rare eye condition called NAION. If severe symptoms develop, it is important to seek medical guidance promptly.
Is semaglutide worth trying for weight loss?
For many people with overweight or obesity who have not found lasting results through lifestyle changes alone, semaglutide is an evidence-based option that brings significant weight loss in both clinical trials and real-world use. The key is using it under medical supervision, with careful logging and open communication with your care team. Personalizing the approach, as with Mingo, makes the process safer and more effective.
Where can I get semaglutide prescribed?
Semaglutide is available only by prescription from licensed healthcare professionals, typically endocrinologists, obesity specialists, or primary care doctors knowledgeable in weight management. Avoid informal routes or online sellers; always use regulated pharmacy supply under supervision to ensure safety and proper dosing.

